Unilateral Nasal Occlusion
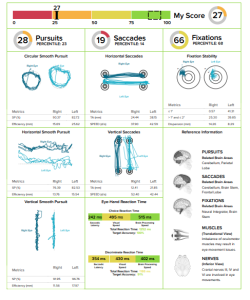
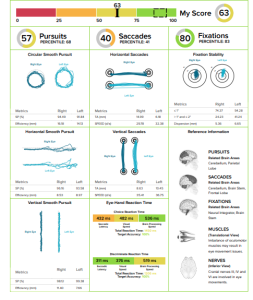
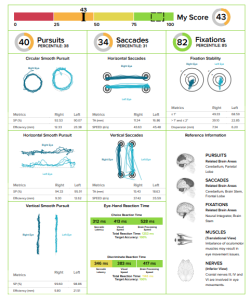
A couple of weeks ago we evaluated a patient that had been diagnosed with a concussion after falling to the ground when slipping her shoes off. She presents with all of the typical high scored symptoms: headache, nausea, visual fatigue, difficulty concentrating, difficulty remembering, but NO SLEEP DYSFUNCTION!!!! Phew, finally one without sleep dysfunction.
Upon observation, we noticed that one eye was naturally more converged than the other. She was actually unaware that her left eye was set this way and reported no history of visual dysfunction. So…instead of using a binasal occlusion to increase bilateral divergence we decided to try unilateral nasal occlusion with the eye that was struggling the most with divergence. After application to the left eye, the occlusion instantly gave the patient mild headache relief and improved eye hand coordination. She was educated to keep it on until she became visually fatigued and then take it off at home. This patient was compliant and reports taking it off a couple hours after her appointment had ended.
In order to keep progressing, we had to get this woman back to work. Along with our inter-professional blog post, she is working with her primary care physician on a return to work plan. She works full time utilizing 2 computer monitors to be effective and efficient in her job, however we all understand how this can cause symptom provocation, eye fatigue, and inhibit concussion recovery. We decided to utilize this unilateral nasal occlusion on her glasses during work hours to see if that would help in getting her eyes to work together and avoid over convergence.
It worked! The patient was able to go from working 3 hours/day last week to 5 hours today (per physician order) with even less symptoms than she had before! She does take the occlusion off after work and continues to demonstrate an increase in visual endurance with eye hand coordination and ocular motor tasks. We plan to continue treating her 2-3x per week until she is asymptomatic and back to work without restrictions.
Unilateral Nasal Occlusion Read More »